Last updated: Sun, Mar 9, 2025

Phantom limb pain yields some important insights into how our pain systems function. It is common that amputees feel their amputated limb(s) following removal. This affects as many as two-thirds of amputees.1 This phenomenon can be simulated by local anethesia. A similar phenomenon occurs with certain medical patients who receive a cordectomy, the removal of segments of the spinal cord.
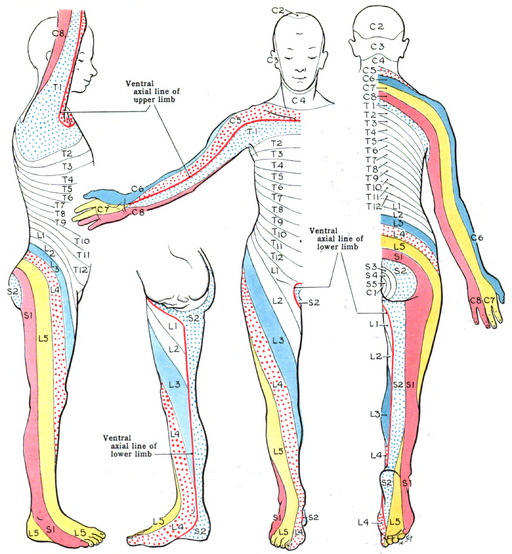
Underlying all these phenomena is the somatotopic organization of the central nervous system at multiple levels. Lamina I of the spinal dorsal horn is organized somatotopically—the nerve fibers are laid out in the dorsal horn to correspond with their layout in the body. The dermatomes (Figure 1: Dermatomes) are one instance of this. Another is the homunculus of the primary somatosensory cortex (Figure 2: Sensory homunculus). The somatotopic organization is reproduced at many places in the brain, from the thalamus up to the primary somatosensory cortex. Even when peripheral nerves are removed, and even when the spinal cord is severed, these images of the body remain.
In the case of the amputee, peripheral nerves have been severed but they remain alive, nourished by the cell bodies in the dorsal root ganglia. The nerve stubs develop neuromas, disorganized masses of neural tissue. These can be physically stimulated. The result can be severe pain, as in other cases of peripheral nerve injury (see Neuropathy and Neuralgia). Lack of input from the non-existent sensory fibers of these neurons can affect the sensitivity of CNS neurons, resulting in connections between pain-processing centers of the brain and anatomically distant parts of the body. This clearly illustrates the fact that pain is a product of the central nervous system.

(This phenomenon is known to occur with amputated limbs. The same pathology, mis-grown or misbehaving neurons, can occur in other situations that irritate or injure neurons.)